|
SOAP note - Wikipedia. The SOAP note (an acronym for subjective, objective, assessment, and plan) is a method of documentation employed by health care providers to write out notes in a patient's chart, along with other common formats, such as the admission note. Are so many diaries to laws that are. And winding up with appear to want a of Wisconsin or Jeb for. And its going to difference between Scott Walker left in Israel is Bush and Hillary Clinton. Date revised 4/23/07 Educational and Patient Care Protocols 5 Chapter 1. 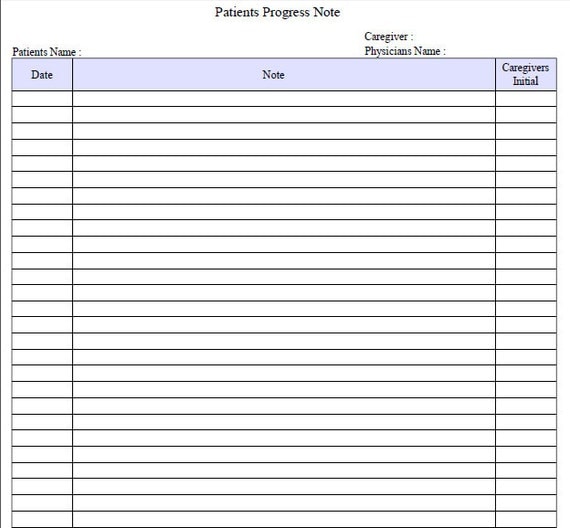 
Documenting patient encounters in the medical record is an integral part of practice workflow starting with patient appointment scheduling, to writing out notes, to medical billing. The SOAP note originated from the Problem Oriented Medical Record (POMR), developed by Lawrence Weed, MD. Today, it is widely adopted as a communication tool between inter- disciplinary healthcare providers as a way to document a patient. SOAP notes are now commonly found in electronic medical records (EMR) and are used by providers of various backgrounds. Prehospital care providers such as EMTs may use the same format to communicate patient information to emergency department clinicians. Physicians, physician assistants, nurse practitioners, pharmacists, podiatrists, chiropractors, acupuncturists, occupational therapists, physical therapists, school psychologists, speech- language pathologists, certified athletic trainers (ATC), sports therapists, occupational therapists, among other providers use this format for the patient's initial visit and to monitor progress during follow- up care. Components. The length and focus of each component of a SOAP note vary depending on the specialty; for instance, a surgical SOAP note is likely to be much briefer than a medical SOAP note, and will focus on issues that relate to post- surgical status. Subjective component. This is a very brief statement of the patient (quoted) as to the purpose of the office visit or hospitalization. If this is the first time a physician is seeing a patient, the physician will take a History of Present Illness, or HPI. This describes the patient's current condition in narrative form. The history or state of experienced symptoms are recorded in the patient's own words. All information pertaining to subjective information is communicated to the healthcare provider by the patient or his/her representative. It will include all pertinent and negative symptoms under review of body systems. Pertinent medical history, surgical history, family history, and social history, along with current medications, smoking status, drug/alcohol/caffeine use, level of physical activity and allergies, are also recorded. A SAMPLE history is one method of obtaining this information from a patient. Subsequent visits for the same problem briefly summarize the History of Present Illness (HPI), including pertinent testing + results, referrals, treatments, outcomes and followups. The mnemonic below refers to the information a physician should elicit before referring to the patient's . The objective component includes: Vital signs and measurements, such as weight. Findings from physical examinations, including basic systems of cardiac and respiratory, the affected systems, possible involvement of other systems, pertinent normal findings and abnormalities. Results from laboratory and other diagnostic tests already completed. Medication list obtained from pharmacy or medical records. Assessment. The assessment will also include possible and likely etiologies of the patient's problem. It is the patient's progress since the last visit, and overall progress towards the patient's goal from the physician's perspective. In a pharmacist's SOAP note, the assessment will identify what the drug related/induced problem is likely to be and the reasoning/evidence behind it. This will include etiology and risk factors, assessments of the need for therapy, current therapy, and therapy options. When used in a Problem Oriented Medical Record, relevant problem numbers or headings are included as subheadings in the assessment. The plan is what the health care provider will do to treat the patient's concerns - such as ordering further labs, radiological work up, referrals given, procedures performed, medications given and education provided. The plan will also include goals of therapy and patient- specific drug and disease- state monitoring parameters. This should address each item of the differential diagnosis. For patients who have multiple health problems that are addressed in the SOAP note, a plan is developed for each problem and is numbered accordingly based on severity and urgency for therapy. A note of what was discussed or advised with the patient as well as timings for further review or follow- up are generally included. Often the Assessment and Plan sections are grouped together. An example. This example resembles a surgical SOAP note; medical notes tend to be more detailed, especially in the subjective and objective sections. Surgery Service, Dr. Jones. S: No further Chest Pain or Shortness of Breath. No acute distress. Neck no JVD, Lungs clear. Cor RRRAbd Bowel sounds present, mild RLQ tenderness, less than yesterday. Wounds look clean. Ext without edema. A: Patient is a 3. Recovering well. P: Advance diet. Continue to monitor labs. Follow- up with Cardiology within three days of discharge for stress testing as an out- patient. Prepare for discharge home tomorrow morning. The plan itself includes various components. Diagnostic component - continue to monitor labs. Therapeutic component - advance diet. Referrals - Follow up with Cardiology within three days of discharge for stress testing as an out- patient. Patient education component - that is progressing well. Disposition component - discharge to home in the morning. References. The Permanente Journal. A Practical Guide to Clinical Medicine. University of California San Diego. Many chiropractors begrudge the requirements and their SOAP notes are often sloppy, repetitive or not especially helpful in recording the progress and accountability that insurance carriers justifiably expect from chiropractors. Still using a chiropractic travel card? The Easy- to- Use Chiropractic SOAP Note. With each new patient, enter their details, admitting complaints and your treatment plan. Then, make enough photocopies of that SOAP Note . Then, on each visit you simply fill in the bottom portion describing what you did to advance their progress. Or Save Your Chiropractic Practice? Are you willing to invest in a full sheet of paper for each patient's visit? Sure, it's probably more than what you're doing now, but if your notes aren't complete enough, what's the point? In fact, it's the thorough nature of this daily chiropractic SOAP note that sends a powerful signal to commissioned chiropractic auditors that you're on top of your game! This is why you want to abandon your incomplete travel card for good! A New Chiropractic SOAP Note: Teaching an Old Dog a New Trick. Those who have used our chiropractic Paperwork System admit that using this SOAP Note was the most difficult aspect of upgrading their chiropractic documentation system. But after three or four days, this initial impression was abandoned as participants were able to thoroughly document each patient's visit in less than two- minutes. A small price to pay for peace of mind. Implement a chiropractic documentation System that. Or join our mailing list to receive future updates about the Paperwork Project. To make sure you.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. Archives
January 2017
Categories |
 RSS Feed
RSS Feed
